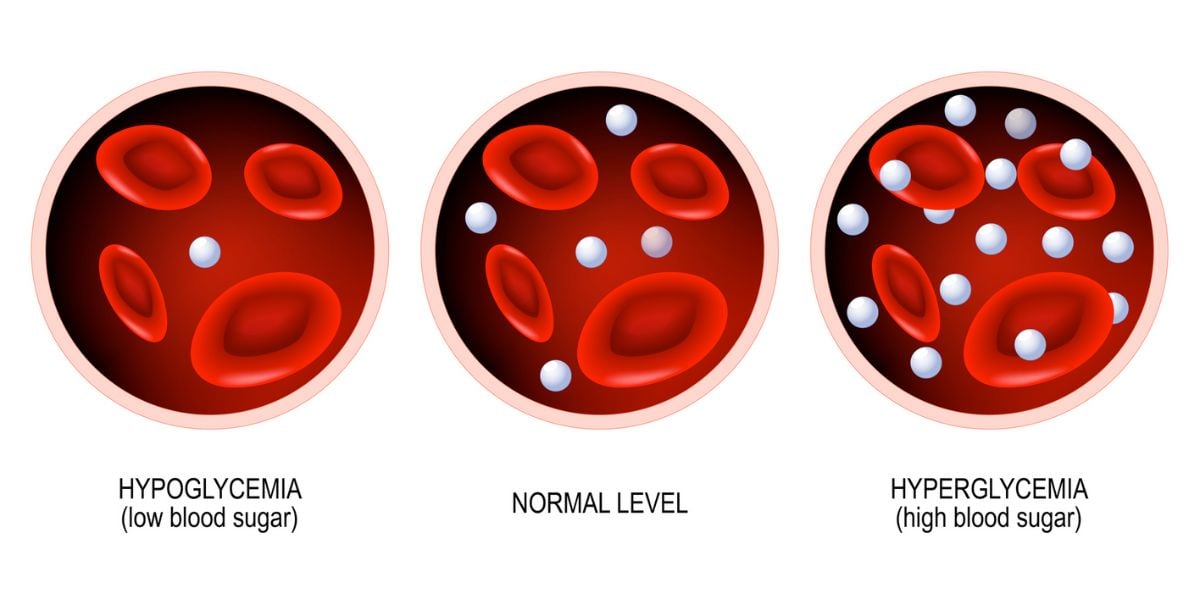
A hypo (hypoglycemia) is triggered when blood sugar levels fall under 4 mmol/L.
Too much insulin or too little food can spark a hypo.
This guide details what hypoglycemia is, how to recognise hypo symptoms, and what to do when you or your child is suffering from a hypo (hypoglycemia).
What are the symptoms of hypo?
Symptoms of hypoglycemia vary from person to person, but people with diabetes should learn to recognise their own signs in order to treat the hypo as quickly as possible.
Some of the most common symptoms of a hypo include:
- Feeling dizzy
- Feeling hungry
- A change in mood
- Feeling sweaty
- Trembling
- Finding it hard to concentrate
What to do if you think you/your child is having a hypo?
If you, or your child, may be having a hypo, it’s often worth checking blood sugar levels as soon as the symptoms are noticed.
However, if testing could delay treating the hypo by more than a minute or two, it is better to treat the hypo immediately and test as soon after as you can.
Someone I know is having a hypo, what should I do?
If someone with diabetes is having a hypo and is conscious, they should initially treat a hypo with 15-20g of fast acting sugary food or drink, such as:
- 5 glucose tablets
- 150 to 200ml of a sugary fizzy drink (eg full sugar cola or lemonade)
- 4 to 5 sugar lumps or teaspoons of sugar
- 150 to 200ml of fruit juice
The priority is to bring blood glucose levels back up to normal as quickly as possible.
Chocolate can be used if little else is available. However, note that the fat in chocolate slows down how quickly the sugar gets broken down, so use sugary foods without fat in where possible.
If someone is unconscious or has a seizure this is a severe hypo. Read more on the symptoms and treatment of a severe hypo
So in the case of serious hypo what should be done?
- The patient should be put into recovery position
- Emergency services should be contacted
- Glucagon should be given as advised
What does glucagon do to a hypo patient?
Glucagon causes blood glucose levels to rise within 10-60 minutes after an injection. Following glucagons, standard instant hypo treatment (glucose tablets, Lucozade, fizzy drinks). Vomiting may occur during the first hour of glucagon injection.
How much glucagon should be given to hypo patients?
Standard glucagon dose is:
- Half a vial – 0.5mg
(Children younger than 8 years) - Full vial – 1mg)
(Children 8 years and above)
Directions for use should be included with the product or your healthcare professional should be able to advise you.
The prefilled syringe should be injected into the glucagon vial, this should then be shaken until contents dissolve, the solution should then be drawn into the syringe with all air removed.
The technique for injection is to inject about ¼ inch into the outer thigh at an angle of 90 degrees.