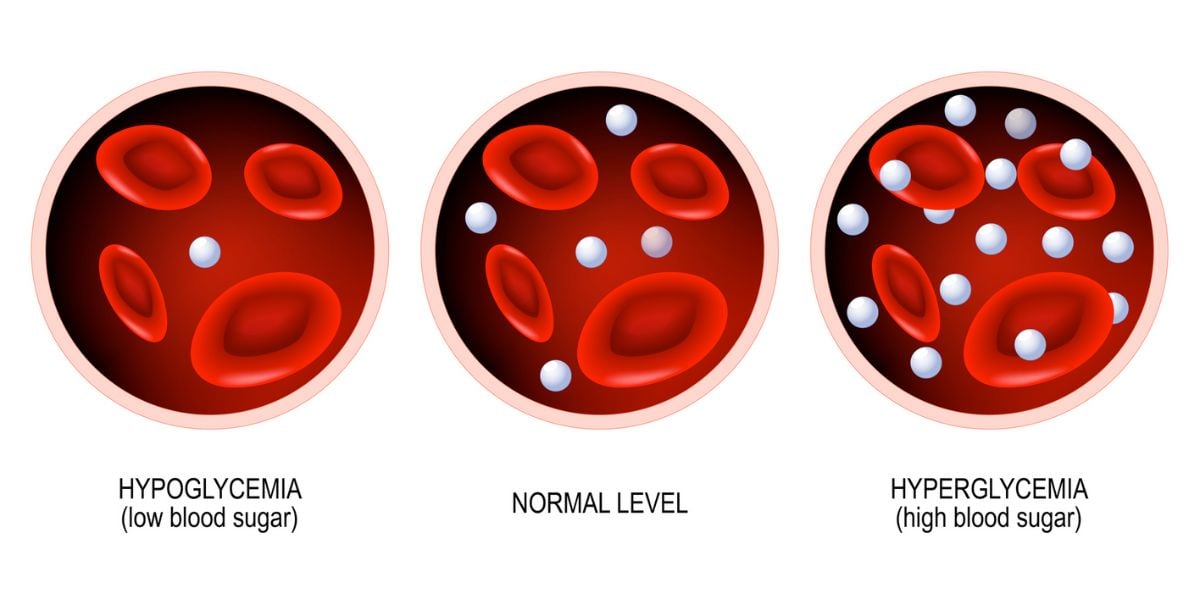
Glucose intolerance is an umbrella term for metabolic conditions which result in higher than normal blood glucose levels – hyperglycemia.
Western lifestyles have seen glucose intolerance become more common year on year.
What conditions are denoted by glucose intolerance?
Conditions which can be considered as glucose intolerance include:
What is glucose intolerance?
Glucose intolerance includes anyone with either impaired fasting glucose (IFG) or impaired glucose tolerance (IGT).
With the World Health Organisation’s definitions for IFG and IGT, glucose intolerance is defined as: [46]
- A fasting blood glucose level of above 6.0 mmol/L or
- A blood glucose level of over 7.8 mmol/L 2 hours after consuming 75g of glucose.
Symptoms of glucose intolerance
The symptoms of glucose intolerance match those of type 2 diabetes:
- Feeling very thirsty
- Dry mouth
- Extreme tiredness
- Blurred vision
- Drowsiness
- Frequent need to urinate
- Loss of muscle mass
The NHS states that not everyone will get these symptoms and symptoms may not be so severe.
Glucose intolerance test
A number of tests can be used to diagnose forms of glucose intolerance.
Test performed to diagnose glucose intolerance include:
Treatment for glucose intolerance
Treatments for glucose intolerance will either require lifestyle changes or a combination of lifestyle changes and anti-diabetic medication
Lifestyle changes involve taking part in regular physical activity, aiming to lose weight, if appropriate, and cutting down on smoking and alcohol as necessary.
If medication is advised, most people will start on a drug, taken in tablet form, called metformin
Some people may need to take additional or alternative medication.