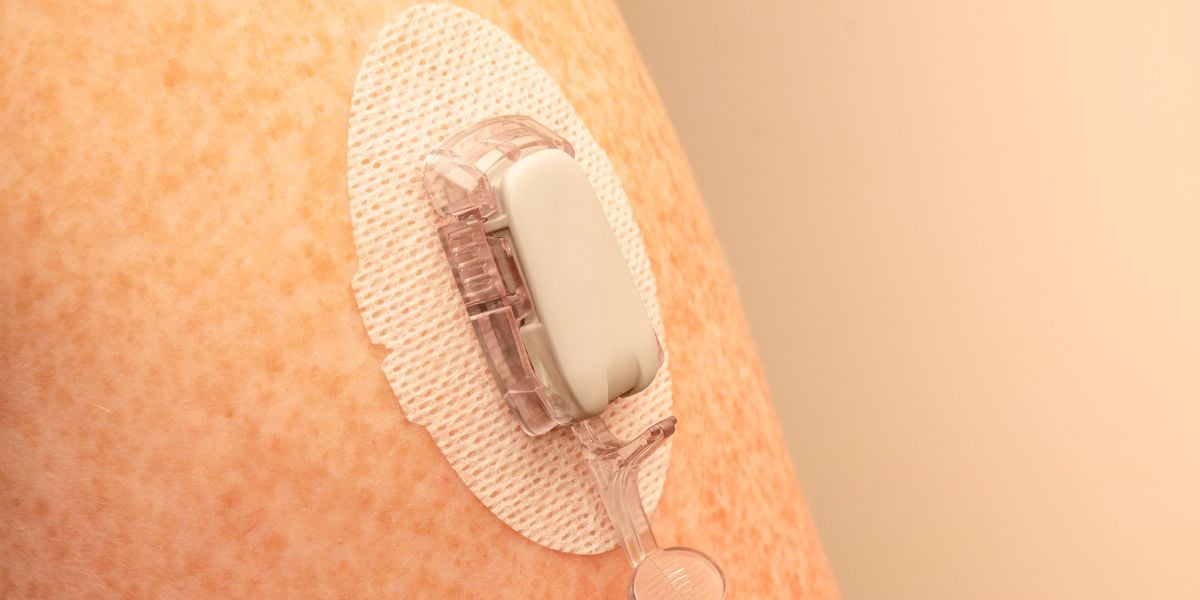
With a blood glucose meter, you use blood to do the test whereas CGM is continuous glucose monitoring.
Continuous glucose monitoring isn’t blood glucose monitoring as the sensors with a CGM machine are placed into your body but not into the bloodstream.
The sensors measure the glucose in your interstitial fluid – the fluid in and around your body’s cells.
The relationship between glucose concentrations in interstitial fluid (ISF) and blood has generated great interest due to the possibility of gaining up to 288 glucose level readings a day without having to do finger pricks
CGM is less invasive
Basically, CGMs are a less invasive technique for measuring glucose. CGM can be used whether you wear a pump or use injections for your insulin delivery CGM systems work 24 hours a day and can include alarms to indicate when your glucose levels are too high or too low.
How do I get continuous glucose monitoring (CGM)?
You can buy a continuous glucose monitor but it is first well worth finding out if you qualify for use of a CGM on the NHS.
NICE recommendations
NICE recommends the use of real-time CGM (rt-CGM) for adults and children with type 1 diabetes as part of an integrated package of care that includes education, self-management support, and regular review. The guidelines specify that CGM can be particularly beneficial for:
- Those who have frequent episodes of hypoglycaemia.
- Individuals experiencing severe hypoglycaemia without warning signs.
NICE advises that pregnant women with type 1 diabetes should be offered continuous glucose monitoring to help manage their glucose levels more effectively during pregnancy.
For children and young people under the age of 18 with type 1 diabetes, CGM is recommended under similar criteria to adults, with a strong emphasis on the need for suitable education and support to ensure effective use.
The guidelines covering children are similar and children should be offered continuous glucose monitoring if they are having frequent episodes of severe hypos or having significant problems as a result of impaired hypo awareness.
Continuous glucose monitoring product guides
Continuous Glucose Monitoring (CGM) is steadily becoming a more in demand way of monitoring diabetes control.
Is it still blood glucose monitoring?
People may assume CGM is continuous glucose monitoring but it is not blood glucose monitoring , as the sensors used are placed into the body but not into the bloodstream.
With a blood glucose meter, you use blood to do the test. With the sensors, they actually measure the glucose in your interstitial fluid, not your blood.
The CGM system can be used whether you wear a pump wearer or use injections for your insulin delivery.
How can CGM help my diabetes control?
By providing as many as hundreds of readings a day, continuous glucose monitoring can help to provide a very clear idea of how long you are spending with high and low glucose levels.
The data continuous glucose monitoring can provide gives a much more detailed and comprehensive picture of control than blood glucose testing can.
One area of uncertainty that commonly exists with standard blood testing is whether highs or lows are taking place when asleep.
Monitoring whilst you sleep
Continuous glucose monitoring has the advantage of being able to provide this information even whilst you’re asleep.
In combination with a detailed food and activity diary, continuous glucose monitoring can offer the chance to make diet, dosage and lifestyle changes to help reduce the amount of time you spend with high or low sugar levels
Continuous glucose monitoring has become a particularly in demand method for monitoring diabetes control in mothers to be with gestational diabetes, as good diabetes control is very important for the development of the baby.
Is CGM as accurate as standard blood glucose monitoring?
The level of glucose in interstitial fluid reacts slower than the level of glucose in the blood.
Therefore, users of a continuous glucose monitoring system should be aware that there is usually a lag of approximately 10 minutes between rises (or drops) in glucose levels compared with the blood.
People using a continuous glucose monitoring system are advised to still perform standard blood glucose tests to ensure that the continuous glucose monitoring device is giving accurate enough results and before making any treatment corrections.