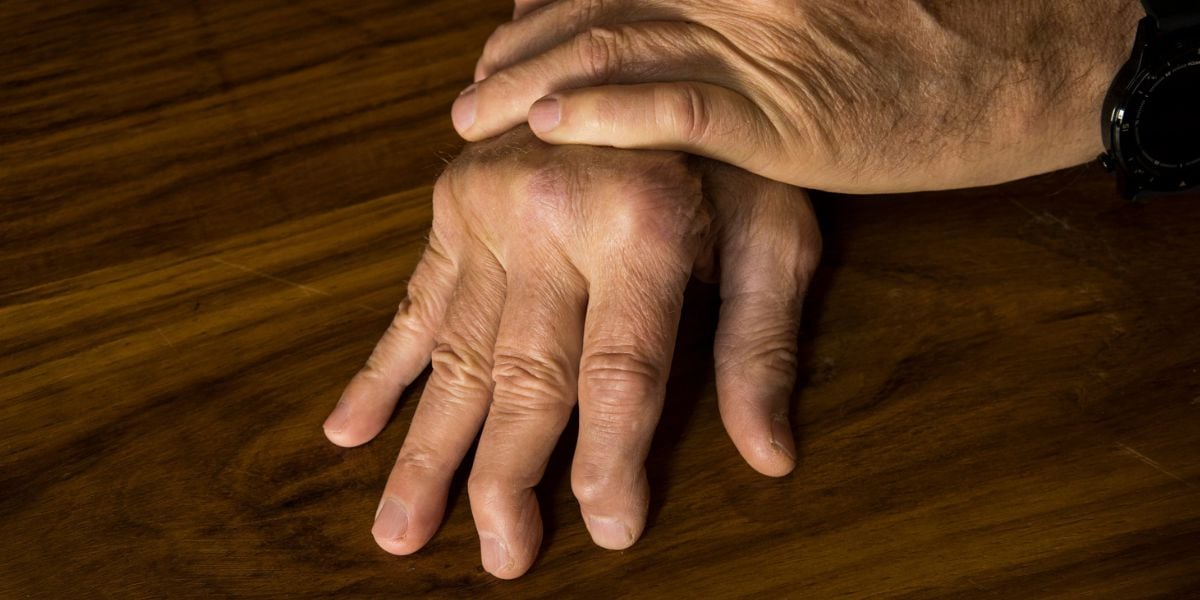
Gout is a form of arthritis (inflammation of joints) caused by high levels of uric acid. Gout can be a painful condition but one that can be managed to reduce the frequency at which gout attacks occur.
Gout is known to affect around 1 in 100 people in the UK and is around four times more common in men than in women.
Research shows that people with gout are significantly more likely to develop type 2 diabetes than people without gout.
Gout and diabetes
A number of research papers have shown associations between gout and type 2 diabetes including a study from Harvard Medical School, published in 2014, which showed gout to be associated with a 70 increased risk of developing type 2 diabetes
A common medication for treating gout, allopurinol, has shown promise for reducing thickening of heart muscle and is currently undergoing testing as a possible medication for reducing risk of diabetic nephropathy (kidney disease).
Symptoms of gout
Gout is characterised by swelling of joints The base of the big toe is most commonly affected by gout. More than one joint may be affected by gout in some people.
Symptoms can come on quickly, with swelling occurring within a few hours. The swollen joint can be very painful and sensitive to touch. During swelling, skin covering the joint may typically turn red and shiny in appearance.
The swelling and symptoms may occur for several days if not treated. Once the inflammation has subsided, the skin on the joint may become itchy and flaky.
Causes of gout
Gout occurs if high levels of uric acid in the blood leads to crystals of sodium urate forming in and around the joints. If these crystals spill into the joint space, this can cause the joint to become inflamed.
Risk factors
High levels of uric acid are more likely to build if you have any of the following risk factors:
- Family history of gout
- Obesity
- Medical conditions that lead to increased uric acid levels
- A diet high in purines – a compound that is broken down into uric acid
Medical conditions which may lead to high uric acid levels include hypoparathyroidism, leukaemia, nephrolithiasis and renal failure.
Foods that are very high in purines include:
- Liver
- Kidneys
- Sardines
- Anchovies
- Sweetbreads (pancreas or thymus) and
- Gravy
Other foods that are relatively high in purines include red meat , oily fish, spinach, asparagus, beans, lentils, oatmeal and wheat bran.
Diagnosing gout
There are other forms of arthritis which can display similar symptoms to gout so tests are needed to confirm whether gout is the cause of inflammation.
The best diagnosis method is to test for presence of uric acid crystals in the affected joint. A needle is pushed in and synovial fluid is collected from the joint and examined, under a microscope, for the presence of sodium urate.
Blood tests, x-rays and ultrasound scans may also be used for diagnosing gout.
Treatment
Treating gout involves measures to prevent gout attacks and treatment when an attack occurs.
A low purine diet is recommend to reduce uric acid from building up. Avoid having foods that are high in purines. Dairy, eggs and most fruit and vegetables are low or relatively low in purines. Aim to avoid alcohol and sweetened foods and drinks as these can increase the risk of gout. Aim to drink 1.5 litres of water a day.
Medications, called urate-lowering therapy (ULT), may commonly be prescribed to reduce levels of uric acid, particularly if gout attacks are frequent or if you have complications of gout such as joint damage or a history of kidney stones.
Common examples of ULT medications are allopurinol and febuxostat.
Treating gout attacks
If an attack of gout develops, treatment will aim to reduce inflammation and pain and may include self-care or medication
Self-care treatment includes keeping the joint rested, to prevent further inflammation or irritation and keeping the joint cool.
You can use an ice pack to cool the joint but don’t put ice directly onto the skin and don’t use an ice pack for more than 20 minutes so as not to damage the skin.
Medications for treating inflammation include:
- NSAIDs (Non-steroidal anti-inflammatory drugs)
- Colchicine
- Corticosteroids
NSAIDs treat pain as well as inflammation but may not be advised if you are at higher risk of heart disease or stroke. Colchicine may lower blood glucose levels so care needs to be taken if you are on hypo causing medication such as insulin, sulphonylureas or glinides.
Corticosteroids may be used to treat severe attacks of gout but can lead to increased blood glucose levels whilst they are being taken.