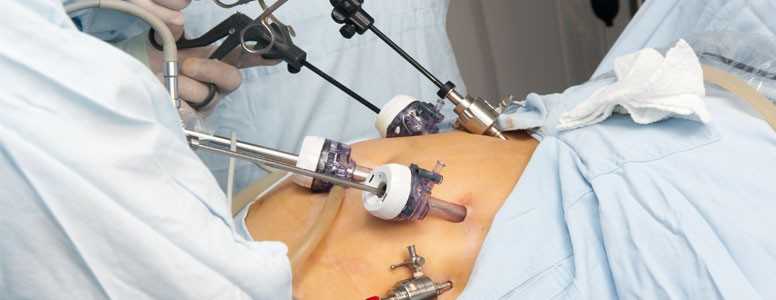
A small study has found that two of the most popular types of bariatric surgery may help restore beta cell function in non-insulin treated type 2 diabetes.
Previous research highlighted that people with type 2 diabetes who underwent RYGB showed resolution of insulin resistance and signs of beta cell rest before significant weight loss had occurred.
Here, researchers followed twenty middle-aged, obese participants with an average HbA1c averaged of 57 mmol/mol (7.4 %) after a Roux-en-Y gastric bypass (RYGB) or sleeve gastrectomy (SG) procedure.
The participants were patients with short-duration type 2 diabetes (4+ years) not yet on insulin, which means that their beta cells still produced some insulin at the time of the study.
Researchers suspended their oral diabetes medications three days prior to assessing markers of type 2 diabetes post-surgery, so as not to distort the effect size of the results.
The first thing they noticed is that their fasting blood sugars had improved with both RYGB and SG, with reductions equalling 2.4 mmol/L and 2.2 mmol/L respectively.
When comparing insulin secretion pre- and post-surgery, which served as an indication of improved beta cell function, researchers reported that it had increased slightly with both RYGB and SG.
The participants also seemed to have regained some degree of insulin sensitivity. The tests showed enhanced insulin response and glucose disposal, especially in the RYGB group.
Three weeks after the surgery, weight loss measurements were taken. The mean weight loss was fairly similar between the two groups, with a reduction in body weight of 8.9 per cent for SG and 8.4 per cent with RYGB.
These findings, presented at the Endo 2017 annual meeting, seem to show that there are short-term improvements in beta cell function with both types of surgery. The question remains as to whether it can be maintained over the long haul.
A randomised, controlled trial (STAMPEDE) suggested that 29% of patients are able to achieve an HbA1c of 42 mmol/mol (6.0%) or less five years after RYGB, while patients have a little less success achieving their HbA1c target with SG long-term.
Researchers now plan to keep following the 20 patients of the current study and are hoping to find similar results, although they predict that RYGB will also prevail.
What's new on the forum? ⭐️
Get our free newsletters
Stay up to date with the latest news, research and breakthroughs.