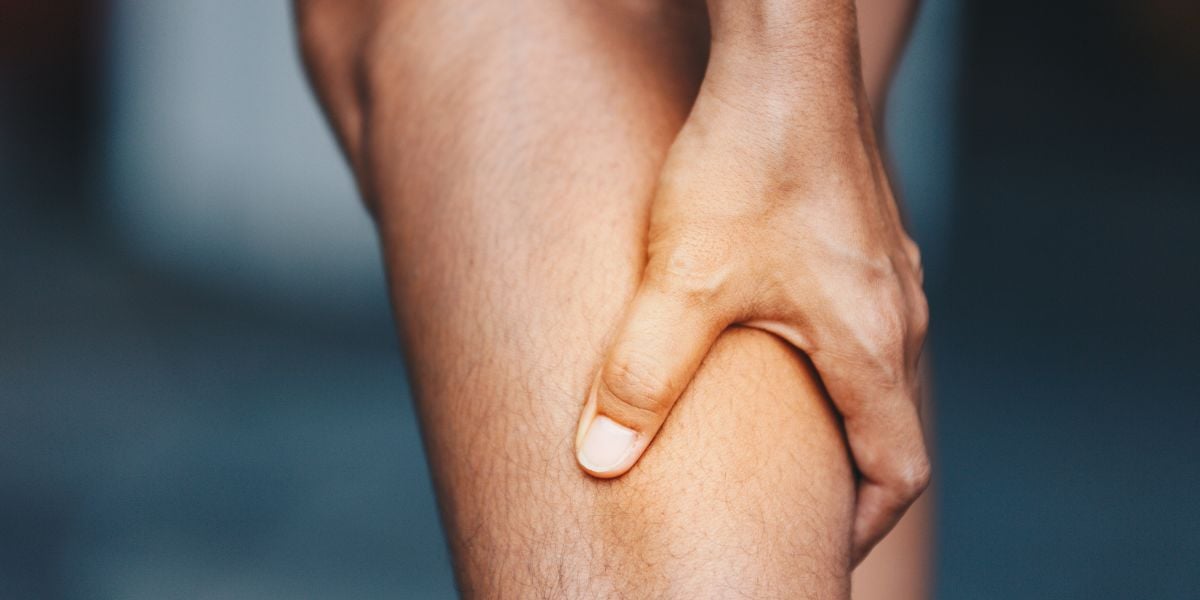
Deep vein thrombosis is the name for blood clots that develop in larger veins such as in the legs.
Thrombosis means blood clot and deep veins are those that lie within the muscle and not visible through the skin. Deep vein thrombosis affects about 1 in 1,000 people each year.
People with diabetes may have an increased risk of DVT, particularly those that have needed surgery or have other inflammatory conditions such as rheumatoid arthritis
Symptoms of deep vein thrombosis
In some cases, deep vein thrombosis may present no symptoms.
If symptoms occur, these can include pain, swelling or aching in the affected leg, often in the calf. You may notice redness or warm skin at the affected part.
Diagnosing DVT
A diagnosis for DVT may include one or more of the following:
- A D-dimer test – a blood test which looks to detect the presence of loose pieces of a blood clot
- An ultrasound scan – which can be used to identify blood clots in deep veins
If the above methods cannot confirm DVT, a venogram may be used. A venogram involves a dye being injected into the foot and X-rays can detect whether the dye is blocked by a blood clot.
What causes deep vein thrombosis?
Deep vein thrombosis is a blood clot and is more likely to occur if we are not able to move around for long periods of time and the blood in the veins slow down. For this reason, deep vein thrombosis has been linked with long distance flights of 8 hours or more.
Being in hospital can increase the risk of DVT as movement may also be limited for long periods of time.
Deep vein thrombosis risk factors
The following factors reflect a higher risk of developing deep vein thrombosis:
- Prolonged inactivity
- Being dehydrated
- Being over 60
- If you are overweight or obese
- Smoking
- If you have existing damage to blood vessels
- If undergoing cancer treatment
- Having inflammatory conditions such as rheumatoid arthritis
Pregnant women and women on the combined contraceptive pill or hormone replacement therapy also have an increased risk of DVT.
Treating deep vein thrombosis
Treatment for DVT will include being given an anticoagulant, such heparin or warfarin, to prevent the blood clot getting worse. Anticoagulants can also prevent the clot from breaking off which can be a life threatening complication of DVT.
Treatment also includes wearing a compression stocking. The stocking is to be worn all day, each day for at least two years to help prevent future clotting developing. You will also be advised to keep your leg raised when resting as this can help the blood to flow from your leg.
Complications of DVT
DVT may result in complications affecting other veins in the leg. This is known as post thrombotic syndrome and its symptoms include pain, swelling, a rash or ulcers on the calf. Speak to your doctor if these symptoms appear.
Pulmonary embolism
A serious complication that can occur following DVT is known as a venous thromboembolism (VTE).
A pulmonary embolism occurs if part of the blood clot breaks off, travels through the veins and gets stuck in the pulmonary artery, preventing blood reaching the lungs.
Symptoms of a pulmonary embolism include chest pain, a shortage of breath, coughing, feeling faint or passing out. Call the emergency services if these symptoms appear as a pulmonary embolism can be severe and can cause death. VTE is estimated to affect 1 in 10 people that have had DVT.