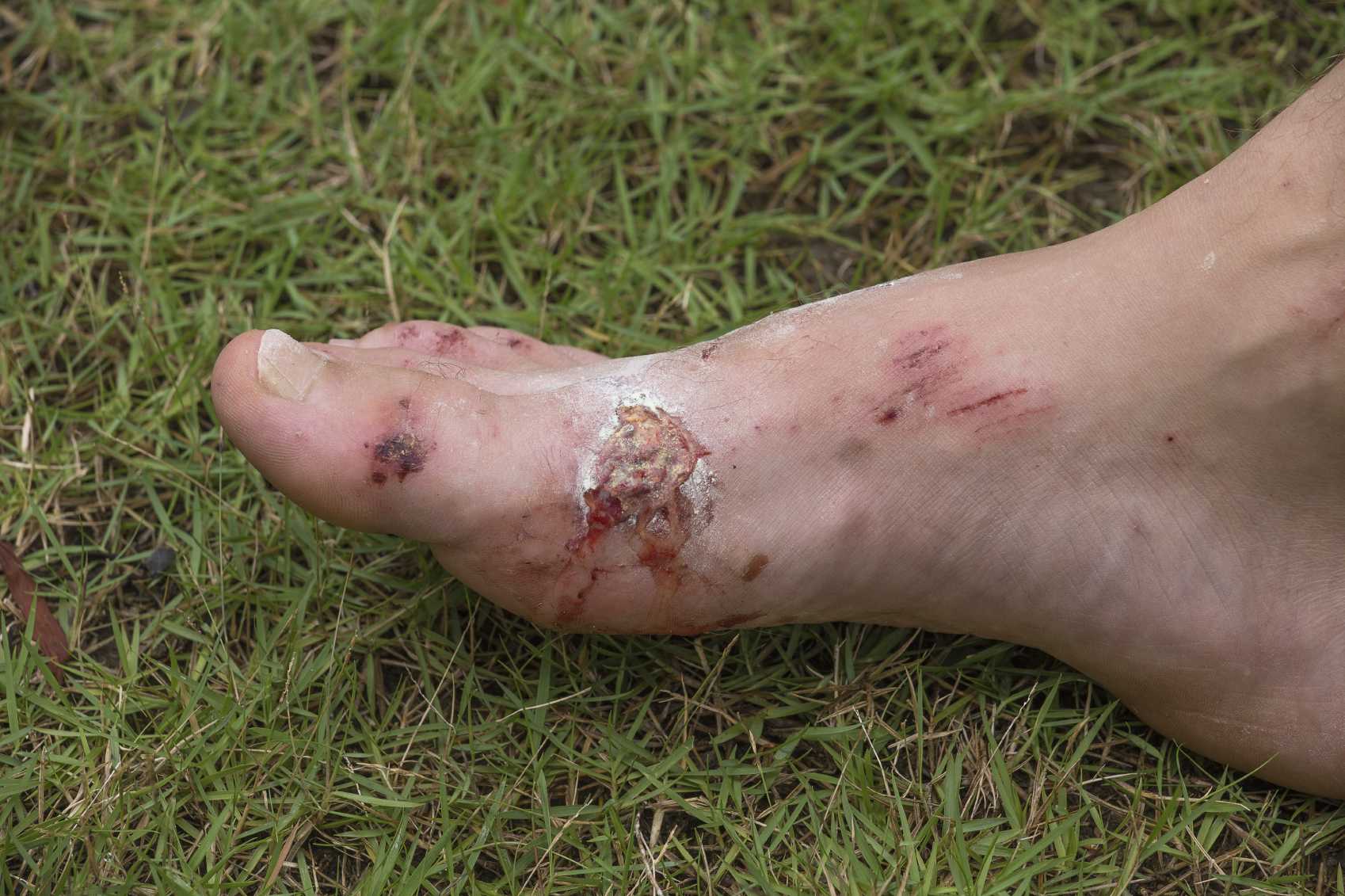
Foot wounds must not be ignored by those of us with diabetes as there are very serious consequences if foot wounds do not heal properly.
A wound which does not heal properly and is left exposed may form a foot ulcer which further raises the risk of an infection occurring.
Indeed, if a wound becomes infected, amputation is a very real prospect if medical attention is not received quickly, as a result of severe complications like gangrene
Gangrene
Gangrene is a serious medical condition that comes in two type, known as “wet” and “dry” gangrene. They are caused by bacterial infections or pre-existing health-issues respectively. Unfortunately, diabetics are at risk of both types.
Gangrene is caused by a lack of blood flow to a certain part of the body, and so diabetes can cause “dry” gangrene by destroying blood vessels. Diabetics can also be at risk of the infections that destroy blood vessels or block off blood flow due to swelling because they have a weakened immune system.
- See here for more information on gangrene, what to do and how to prevent it
Signs of foot wounds
Foot wounds are any break in the skin and therefore include any of the following that causes skin to be lost or open out:
- Cuts
- Grazes
- Blisters
- Cracked skin
- Loss of skin following a corn or callus
- In grown toenails pressing against the surrounding skin
If you notice any signs of wounding, or any of the above signs that can lead to wounds, make an appointment to see your GP.
If a wound has gone unnoticed or heals slowly, the affected area may grow larger and become a foot ulcer. Having a foot ulcer increases the risk of infection so it’s important to notify your GP or podiatrist as soon as possible.
Symptoms of infection
The following symptoms at the site of the wound may indicate that the foot has become infected:
- Swelling
- Reddening of white skin, darkening of brown or black skin
- You may experience increasing amount of pain
- Skin feels warm to the touch
- The appearance of pus
Infection may be accompanied by other symptoms including:
- Having a high temperature
- Swollen glands
- Feeling lethargic and unwell
If you notice these signs arrange to see your GP or health team with a day and if this is not possible, visit your A&E (Accident and Emergency).
Causes
Cuts, grazes and blisters are more likely to occur if you don’t wear comfortable fitting footwear or if you walk around bare foot.
Damage can also occur from activities including:
- Dropping objects on your feet
- Stubbing your feet
- Being trod on
- Burns or scalding from hot water or heaters
- Accidents when clipping toenails
People with diabetes need to extra careful because diabetes can affect the sensory nerves in the feet which can mean suffering wounds without noticing.
If wounds are not well protected, there’s a greater risk of infection and another key factor is that wounds tend to heal more slowly in people with diabetes
Complications
If wounds do not heal properly, the wounds may form an ulcer where the surface of the skin breaks down over an area of the skin leaving the tissue underneath exposed.
It’s important that foot ulcers are treated immediately as infection can set in which can significantly raise the risk of amputation if it causes gangrene or spreads to infect the bone.
Treatment
If you develop a wound, it’s important to:
- Clean the wound in a bowl or warm but not hot water.
- Cover the wound with a sterile wound dressing or bandage to prevent any infection getting in.
- Clean the wound and change the dressing or bandage each day.
- Ensure you do not aggravate the wound and limit how much your walk on it.
- Notify your health team, who will be to advise you on any other treatment or precautions you should take.
Let your doctor know if there is, or could be, an object in the wound, such as a splinter or piece of debris such as glass or metal.
Treatment for infected wounds
If the wound has become infected you need to seek medical help immediately. An infected wound can be treated with antibiotics but people with diabetes may often require additional care to help ensure the wound heals properly.
If you cannot see your GP or a member of your health team within a day, go to your nearest A&E (Accident and Emergency).
Preventing wounds and infections
You can help to minimise the risk of wounds occurring by wearing comfortable, well-fitting shoes which will help to reduce the chances of developing blisters, calluses or other foot problems such as hammer toes.
Avoid walking around bare foot to prevent the risk of cuts, burns or grazes occurring. Remember that if you have nerve damage (neuropathy), you may not feel pain should a foot injury occur.
Check your feet each day for signs of damage or any changes in feeling or appearance in your feet. If you notice something different, notify your doctor. Don’t wait to see if things get better as this can sometimes lead to getting the treatment you need too late.
Try to maintain good control of blood glucose levels as well as this will help any wounds you’ve suffered to heal more quickly.