An increasing number of people choose to reverse gastric band weight loss surgeries and the procedure is losing in popularity, according to a new US study.
Band surgery is fast becoming the next front in the battle against obesity to help with weight loss and reduce risks of insulin resistance, high blood pressure, fatty liver, type 2 diabetes and other long-term complications.
Scientists believe that the body starts to repair itself as the weight falls. However, research has yet to establish whether immediate improvements from weight loss surgery justify altering someone’s digestive system.
Relatively few studies have followed patients for more than two years after surgery and studies have shown that some may regain weight and still develop complications that aren’t detected until later.
The data provides reason for both encouragement and caution. It shows that the weight loss is significant during the first year but slows over time, with the body mass index (BMI) eventually leveling off in year two.
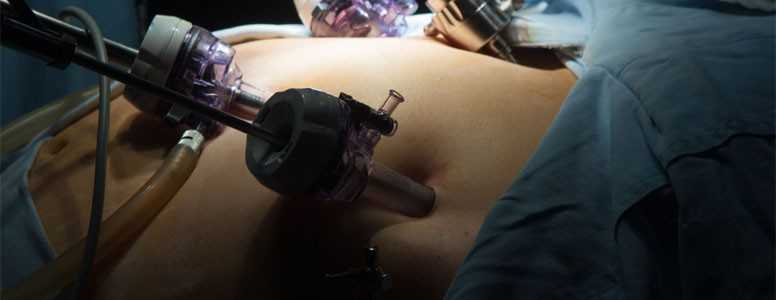
Here, researchers from the University of California, Irvine School of Medicine have focused on a particular type of weight loss surgery called laparoscopic adjustable gastric banding.
This procedure involves wrapping an inflatable belt around the upper portion of the stomach, sometimes sewn in place, that reduces the amount of food it can hold.
Like a gastric bypass, a lap band procedure can be reversed in theory, but this means a possible weight regain and can be dangerous. Going back to reoperate on tissue increases risks of bleeding and damage to structures being repaired.
That’s over and above complications associated with any surgery, like blood clots, infection and injury to adjacent tissues. Getting suture lines to heal properly after a repeat operation can be challenging as well.
Looking at national registers in the US, researchers found that a total of 28,202 patients underwent a lap band procedure from 2007 to 2015. During that same period, 12,157 people had gastric bands removed.
According to what the study team reported in the Journal of the American College of Surgeons, the downward trend in putting bands in started around the year 2013.
In the study, procedures to remove or adjust gastric bands were associated with longer hospital stays, sometimes in intensive care, and a higher complication rate.
From the data, patients most often choose to have it taken off because they can’t tolerate the device being tightened or because they didn’t lose enough weight and opt for an alternative surgery, such as the newest sleeve gastrectomy.
Overall, more research is needed to explain whether bands are removed after complications or to switch to a replacement surgery with better longer-term outcomes.
What's new on the forum? ⭐️
Get our free newsletters
Stay up to date with the latest news, research and breakthroughs.