The discovery and advancement of insulin as a diabetes treatment can be traced back to the 19th century.
Research into the development of insulin has driven scientists to take significant steps towards understanding human biology and a number of Nobel Prizes have been awarded for research into the hormone.
- 1869
Paul Langerhans, a medical student in Berli, discovers a distinct collection of cells within the pancreas. These cells would later be called the Islets of Langerhans.
- 1889
Oscar Minkowski and Joseph von Mering remove a dog’s pancreas to study the effects on digestion. Flies are found to be feeding off the dog’s urine, which is shown to contain sugar.
- 1901
Eugene Opie discovers that the Islets of Langerhans produce insulin and that the destruction of these cells resulted in diabetes
- 1916
Romanian professor Nicolae Paulescu develops an extract of the pancreas and shows that it lowers blood sugar in diabetic dogs. World War I prevents the experiments from continuing and it is not until 1921 that Paulescu publishes evidence of the experiments. [81]
- 1921
Dr Frederick Banting and medical student Charles Best perform experiments on the pancreases of dogs in Toronto, Canada. Professor John Macleod provides Banting and Best with a laboratory to carry out the experiments.
When the pancreases are removed the dogs showed symptoms of diabetes The pancreas was then sliced and ground up into an injectable extract. This is injected a few times a day which helped the dogs to regain health.
Given the early success, Macleod wants to see more evidence that the procedure worked and provides pancreases from cows to make the extract which is named ‘insulin’.
Bertram Collip, a biochemist, joins the research team to provide help with purifying the insulin to be used for testing on humans. Banting and Best clearly had confidence in the insulin as they were the first humans to test the insulin by injecting themselves with it which caused them to experience weakness and dizziness, signs of hypoglycemia
After the group had experimented enough to gain an understanding of the required doses and how best to treat hypoglycemia, their insulin is deemed ready to be tried on patients.
- 1922
A 14-year-old boy with type 1 diabetes called Leonard Thompson is given the first medical administration of insulin. A second dose purified by James B. Collip is successful. Leonard lives for another 13 years. Previously patients with type 1 diabetes would be put onto starvation diets and would have only months to live. Leonard lives another 13 years before succumbing to pneumonia.
As news of insulin’s success spread, Banting and Best begin receiving letters asking for help for others with type 1 diabetes. Banting and Best improve their techniques for the production of insulin and Eli Lilly becomes the first insulin manufacturer.
- 1923
Banting and Macleod are awarded the Nobel Prize in Physiology or Medicine. Banting and Macleod, however, feel Best and Collip were equally eligible and shared their prize money with their two colleagues. [82]
- 1936
Danish physician Hans Christian Hagedorn discovers the action of insulin can be prolonged with the addition of protamine.
- 1950
NPH, an intermediate acting insulin , is marketed by Danish pharmaceutical company Novo Nordisk.
- 1955
Insulin is sequenced by British biochemist Frederick Sanger, and is the first protein to be fully sequenced. In 1958 Sanger receives the Nobel Prize in Chemistry for his research.
- 1963
Insulin becomes the first human protein to be chemically synthesised.
- 1978
Biotechnology firm Genentech uses recombinant DNA techniques to produce synthetic “human” insulin. Insulin is the first human protein by to be manufactured through biotechnology.
1982Synthetic insulin is renamed ‘human insulin’ marking it as distinct from insulin derived from animals Human insulin has the advantage of being less likely to allergic reactions than animal insulin. Humuli, manufactured by Eli Lilly, becomes widely available through the 1980s.
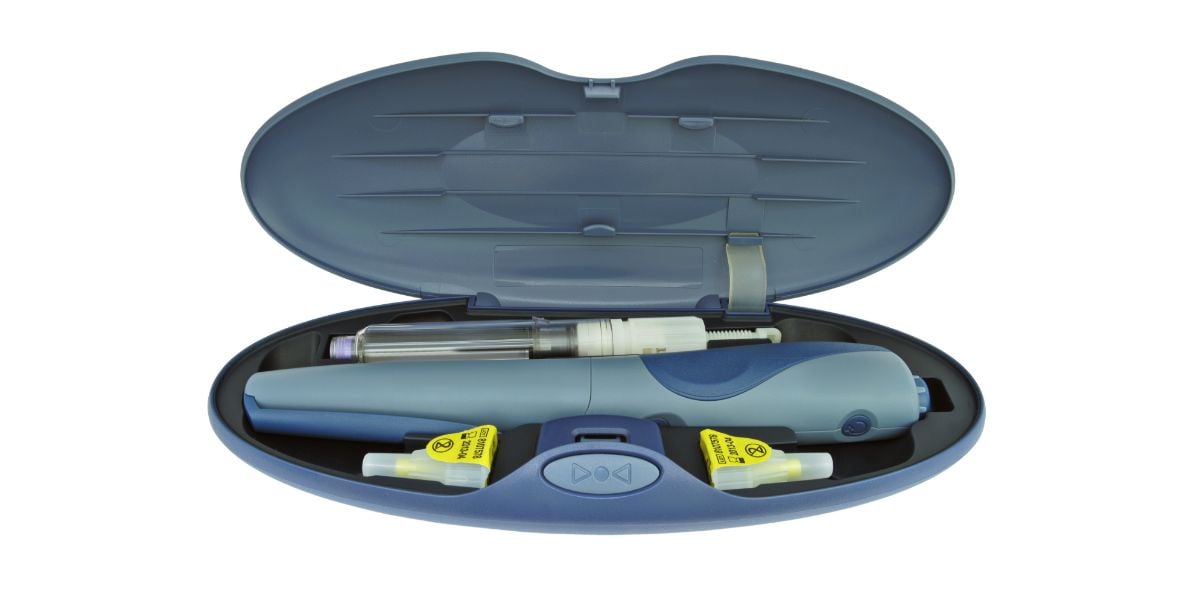
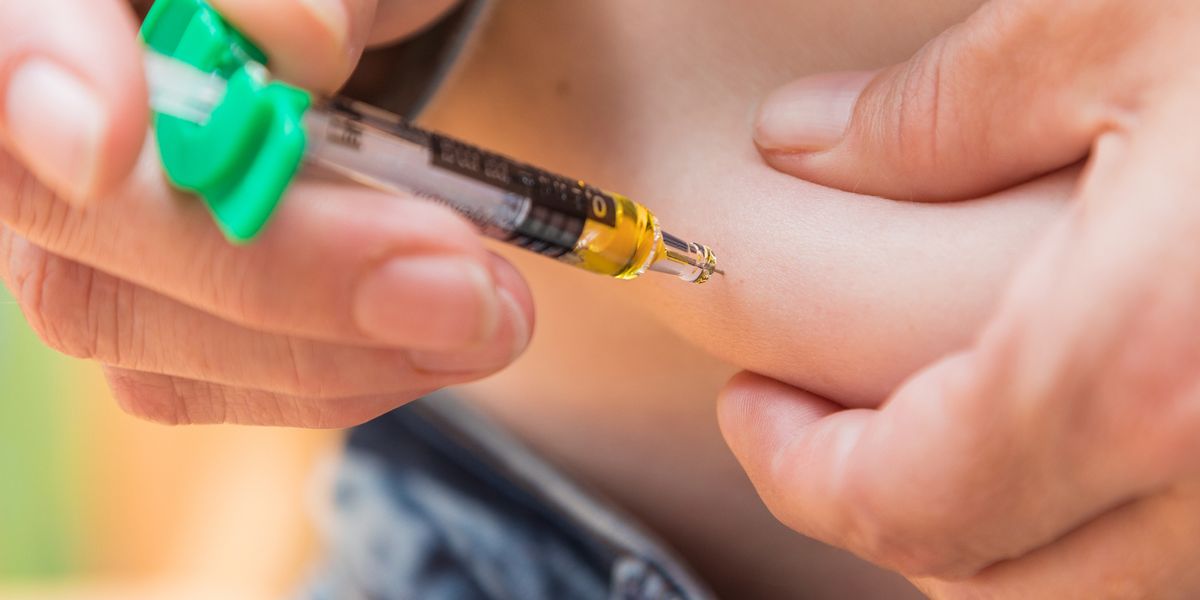
1985Novo Nordisk introduces the Insulin Pen delivery system.
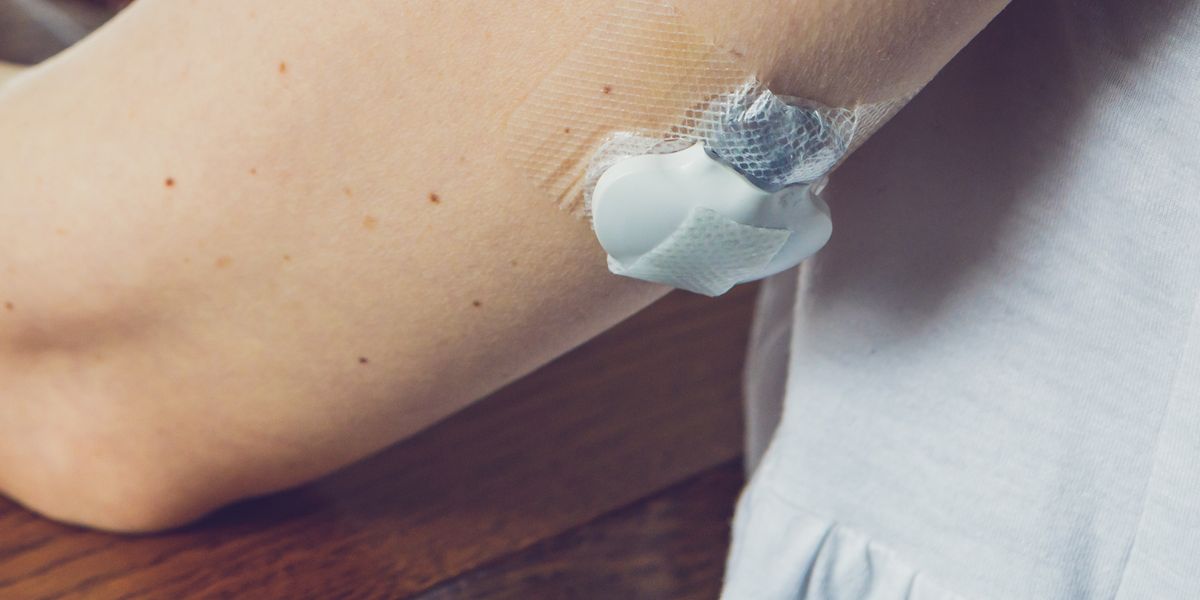
1992Medtronic releases the MiniMed 506 insulin pump, which delivers meal bolus memory and daily insulin totals.
1996Eli Lilly markets the analogue insulin lispro under the trade name Humalog. Analogue insulin is a genetically modified form of insulin whereby the amino acid sequence is altered to change how the insulin is absorbed, distributed, metabolised and excreted [83]
2000More than 470 patients with type 1 diabetes receive islet cell transplantation during the next five years. The procedures help diabetes patients become free from insulin providing they take immunosuppressant drugs.
2013The University of Cambridge develops an artificial pancreas that pairs the technology of an insulin pump with a continuous glucose monitor.
2015Dr Edward Damiano introduces the iLet , which he calls “a bridge to a cure”. The device is a bionic pancreas that delivers both insulin and glucagon every five minutes as required.