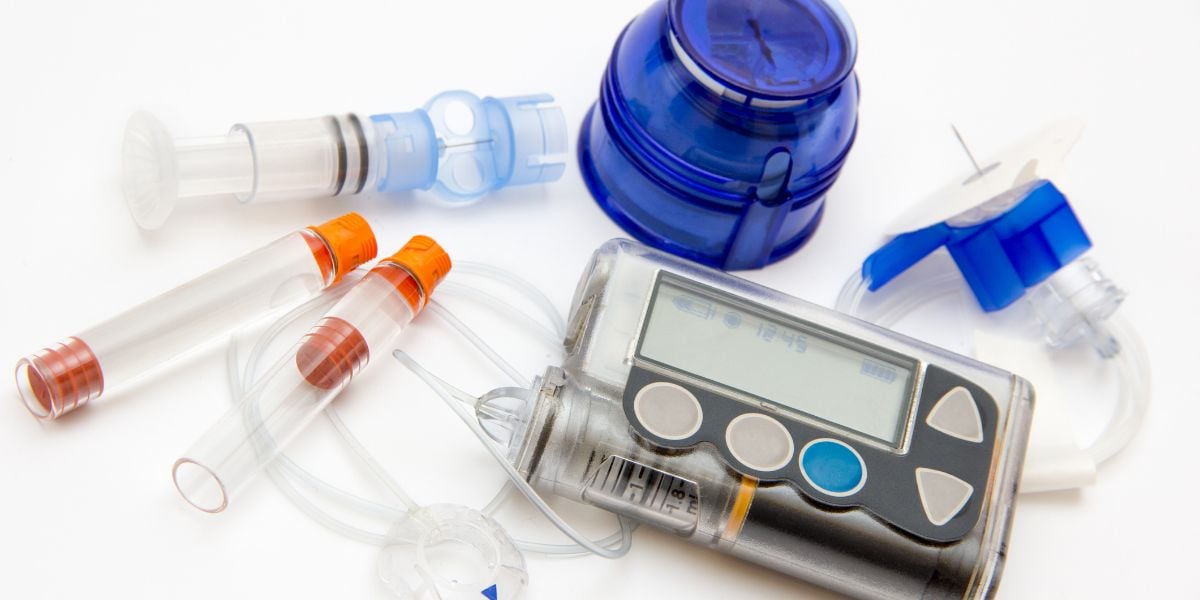
Starting insulin pump therapy can feel like stepping into a new world but many have found going onto an insulin pump well worth the initial effort.
This is a guide to starting insulin pump therapy, the equipment you’ll require, looking after your pump and adjustments to your routine.
Starting insulin therapy
When you first go on a pump you should have an induction day at your local clinic.
For this you are likely to be in with a group of others also going on an insulin pump for the first time and you are also likely to be going on the same pump, as healthcare clinics tend to have contracts with one supplier.
This is an advantage as it means you’re all in the same boat. In the presence of a nurse or other healthcare professional you’ll take the pumps out of their boxes and start to get familiar with all the equipment involved as well as how the pump works
Pump equipment
The amount and variety of kit is different for each pump modal, but they all run along the same lines. Initially, this is the part that is the most baffling.
Medical kit can often seem intimidating, not least because if often involves needles
Becoming familiar with your pump
You will quickly become familiar with it when you start using it and you will have plenty of literature to refer to should you need a reminder of how to use a certain piece of the kit.
You should also be given the number of someone to ring at the clinic as well as a number of the supplier, so if you really do run into trouble you can get advice 24-hours a day, and 7 days a week.
Don’t forget your needles
If you’re going on a pump you may think you are leaving needles behind – which to a great extent you are. However, in order to get an infusion set put under your skin, you will need to use an inserter which will have a needle in it to help pierce the skin.
Infusion sets
Some infusion sets can be put in manually, which means using a needle too, but once the infusion set is in place the needle is withdrawn and thrown safely away. In this way you replace what is probably a regime of four injections a day with one every three days, which is how often you will be replacing your infusion set.
You will be shown how to fill the disposable reservoir with insulin , put the infusion set onto one end of the reservoir, with the reservoir then being put inside the pump. You will then prime it – checking that the insulin is flowing through it correctly – before inserting the infusion set.
The pump itself
While becoming familiar with infusion sets and how to insert them, you will also be getting used to the buttons on the pump and what they do. The general move from multiple daily injections – usually one long-acting insulin per day plus a short-acting insulin with meals – is easy to understand.
Although you take just one insulin, a short-acting one, you replace your long-acting insulin with ongoing infusion of small amounts of the insulin all day long.
This is called your basal rate , which can be adjusted to reflect normal variations in blood glucose levels through the day.
For example, most of us need more insulin in the mornings, part of a natural cycle called the Dawn Phenomenon
Then you replace your meal-time doses with what is called a bolus – it’s simply a dose delivered by the pump that you plug in yourself based on what you are about to eat.
You will amend your pump settings, such as inputting your basal rates, with your healthcare professional based on your existing insulin doses and you will be given advice as to what boluses to give.
You will always need to keep an eye on basal rates and boluses as they may need to be amended as time goes on.
Changing to a pump
The change to your regime will primarily involve fitting in changing infusion sets – every three days you will need to get all the bits together to change over from one set to another. For the first few times you will need to concentrate.
As you only do an infusion set change every three days, it’s easy to forget the detail and plunge into doubt that you are doing the right things in the right order. Take it slowly, and you’ll get there.
Changes to your routine
As you begin to use your insulin pump, you’ll find that you begin to adapt your daily routine.
No more needles?
Not quite – different kit. Some will come from your GP, some either from the clinic or the supplier of the pump. You will be advised by your care team.
No more insulin pens?
Yes, but keep one spare just in case – pumps are extremely reliable, but life can throw us some surprises. Best practice is that it’s better to be safe than sorry, so keep you old pen to hand.
No more insulin cartridges?
No, instead it’s back to bottles of insulin so you need to change your prescription at your GPs.
No more blood testing?
No, still blood test pretty much as before, perhaps with additional testing when you change an infusion set.
No more dose adjustment?
Actually, the basic ideas of how you run your diabetes do not change with a pump, and you still need to be aware of how your doses vary over time.
You will need to assess your basal rates and also your boluses.