Peter Shaw’s father was an aircraft engineer and his family was stationed overseas in Brunei when Peter was diagnosed with diabetes
He recalls, “The only injections I’d had before then had been immunization jabs which I’d really hated having. I was 10 when I was diagnosed and my main memory is being told I was going to have injections for the rest of my life. I was truly terrified of the thought.”
“I also remember that Type 1 diabetes was so rarely seen that the doctors at the hospital were calling back to colleagues in the UK for tips on stabilizing a newly diagnosed T1, as most hadn’t studied this since training.”
Diabetes in the 1980s
This was in the mid-1980s and as there were issues starting to affect the regio, combined with Peter’s age, educational needs and diagnosis of diabetes, the family decided to return to the UK.
Better care in the UK
“The care was miles better in the UK,” says Peter, the care received in Brunei was excellent, it just took them a while to get up to speed “I was seen by a paediatrics team at Horsham Hospital. But back then, blood test meters were almost the size of laptops and lancing devices were like something from the French Revolution! I had a very early Ames Autlolet but my mum had to do the lancing. The blood test meter was a Glucometer, also by Ames, that my dad had to get imported via his company from the USA as they simply weren’t available. It was hard work for those around me.”
OmniPod insulin pump
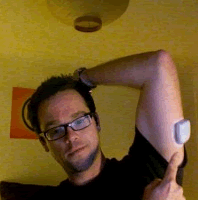
Today Peter is on an OmniPod insulin pump that has an on-board blood test meter. He chose the OmniPod because of his involvement in kite surfing. He is vice-chairman of the British Kite Surfing Association and regularly spends extended periods of time in a wet suit. “As I do a lot of watersports, I needed a pump that did not have tubing,” explains Peter.
“I can get a wet suit on over the pod without pulling it out and tell it what to do with the handheld device. I have no worries about tangling or snagging. It’s waterproof, although in all honesty nothing is really sea-water proof so in this respect, the pods 3-day life span is a boon as they don’t have to survive past that time.
I put the PDM in a watertight case when I’m not using it. I use a Multiclix finger-pricker as I don’t have to handle any sharps and it’s reliable, solid and painless but could do with being smaller. It’s a great bit of kit. It’s all so much better than in the old days!”
Peter has learned from experience that testing after the first 30-40 minutes on the water is key, as this is the window when adrenaline (and being cold) can mask hypo symptoms “I force myself to come in and test after the first half hour and then I know I’m okay for another hour or so. After that, I just have to be careful when I start to tire as that can also cover symptoms.
And I never go on the water without a couple of sachets of glucose gel stashed in my harness!”
Active and healthy!
Despite an active (and relatively healthy) lifestyle and constant carb counting , Peter says that there has been a slow decline in his control over the last few years which was the main reason for the switch to pump-therapy.
He had an HbA1c of 5.2 in 2007 and it’s now 7.2 – still a very respectable level although it is higher.
“My care team at the hospital have been great, especially my diabetes specialist nurse. They’re behind me all the way. I’m hoping to go on a CGM ( continuous glucose monitoring ) trial too. I’ll give anything a go if it helps me live the lifestyle I want.”









